Ophthalmic Imaging
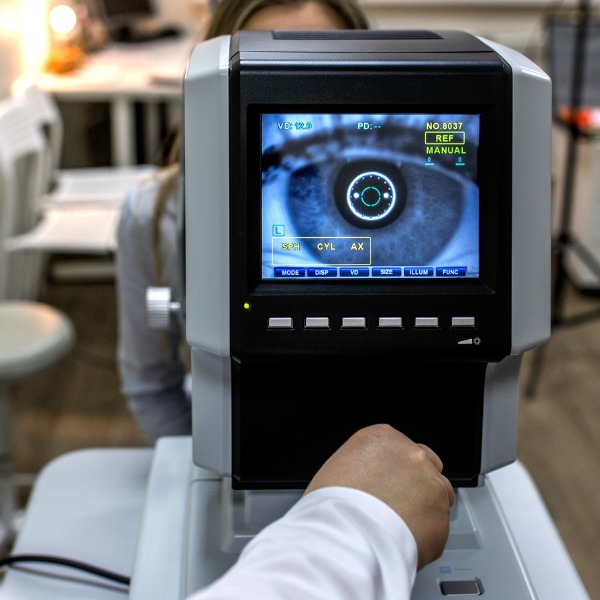
Ophthalmic imaging equipment (mingazitdinov, iStockphoto)

Ophthalmic imaging equipment (mingazitdinov, iStockphoto)
How does this align with my curriculum?
| Grade | Course | Topic |
|---|
Learn about the history, function, uses, benefits and risks of ophthalmic imaging as a medical imaging technology.
Ophthalmic Imaging
How well we see depends on the health of our eyes. The study of eyes is called ophthalmology, which comes from the Greek words ophthalmos, meaning ‘eye,’ and logia, which means ‘the study of’.
The Fundus
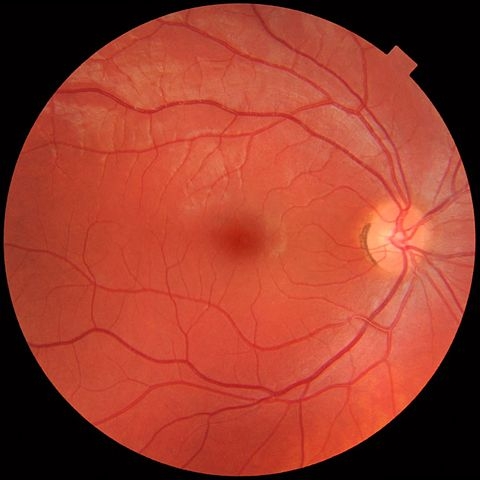
Have you ever seen a photograph in which a person has ‘red-eye?’ The Red-eye effect occurs when light from the camera flash reflects off the back of the eye. The back of the eye is called the fundus. The fundus includes the retina, fovea, optic disc and macula. The many blood vessels in the fundus cause more red light to be reflected, which is why we sometimes get that red-eye in photos. We tend to get the worst red-eye when pictures are taken in a dark room because our pupils are wide open. So how can you avoid getting ‘red-eye?’ Don’t look directly at the flash! A healthy fundus is important to overall eye health. Eye doctors can see and record images of your fundus using ophthalmic imaging tools.
Ophthalmoscope
The health of the eye is very important for quality of life. The tools described here, and other imaging tools used by healthcare professionals, can help catch diseases early enough to treat or prevent damage to the eye and vision. The ophthalmoscope was one of the first devices invented to look into the eye and help understand how it functioned.
History
The first ophthalmoscope was made in 1847 by Charles Babbage. It was independently invented in 1851 by Hermann von Helmholtz. Within 50 years of the first ophthalmoscope, there were at least 140 different models. Several examples are shown below. Early ophthalmoscopes used a candle for their light source. Oil and gas lamps were also popular light sources before Thomas Edison invented the incandescent bulb in 1879. Initial designs that used light bulbs only worked for a short period. Nowadays, handheld battery-operated devices work for a long time with very little energy consumption.

How it Works
An ophthalmoscope has several parts. The light is focused and directed into the patient’s eye with lenses and mirrors. The light that is reflected from the back of the eye is directed through a one-way mirror into the observer’s eye (often the optometrist). If the image is blurry, a focusing lens can be used (just like in eyeglasses) to make images clearer. Handheld ophthalmoscopes can see only a small part of the fundus at once.
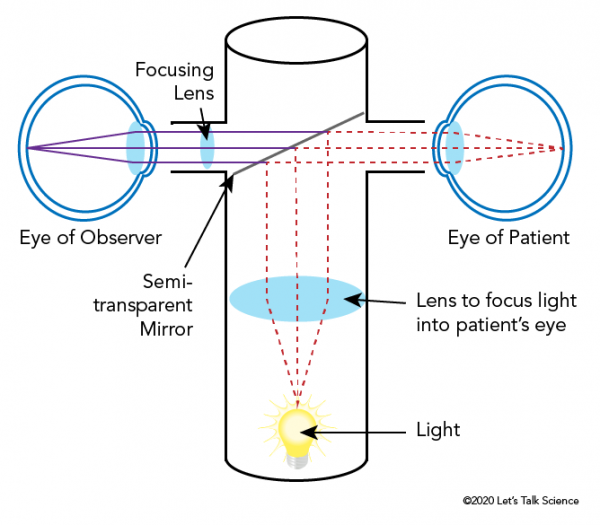
Modern Ophthalmoscopes
Fundus cameras are ophthalmoscopes that can see a larger area of the fundus as well as take pictures.

Before these digital cameras, pictures had to be recorded on film. A Scanning Laser Ophthalmoscope (SLO) uses a single wavelength of light from a laser instead of a light source like a light bulb. The laser beam is focused on a small spot and motorized mirrors move the spot across the fundus very quickly. A computer stores data from every point and then makes a 2D picture. Optical coherence tomography (OCT) takes pictures at many depths in the back of the eye (like the slices of a CT scan) and then creates a 3D image.
Uses
Diseases can change the way the fundus looks and therefore the way we see. Medical professionals examine the fundus for signs of swelling of the retina, changes in blood vessels and damage to the nerve tissue as these are signs of eye disease. The shape and colour of the optic nerve can help diagnose glaucoma. Glaucoma is a disease in which damage to the optic nerve can lead to blindness (B). Complications from diabetes can cause damage to the retina called diabetic retinopathy (C). Diabetics need fundus examinations regularly to catch signs of diabetic retinopathy so it can be corrected with surgery before it causes permanent vision loss.

Benefits & Risks
Ophthalmic imaging is a very safe technique. Although shining bright lights and lasers into your eye can be harmful, the imaging tools described here are designed and tested to be very safe and effective when used by professionals.
Learn More
This article by the Computer History Museum is a brief biography of Charles Babbage, who invented the ophthalmoscope, failsafe quick release couplings for railway carriages, multi-colored theatre lighting, an altimeter, a seismic detector, a tugboat for winching vessels upstream, a 'hydrofoil' and an arcade game.
References
mrcophth.com. (n. d.) The Ophthalmoscope.
Opthalmic Photographers' Society. (n. d.) Ophthalmic Photography. opsweb.org.